Don’t Skip These Screenings
Health Screenings You Shouldn’t Skip in Your 40s and 50s
Turning 40 or 50 often feels like a milestone—and it’s also the perfect time to prioritize preventive health. Regular screenings can detect problems early, when they’re most treatable, and keep you on track for a healthier future.
Here’s a practical checklist of the screenings you shouldn’t skip:
✅ Blood Pressure & Cholesterol
- Why it matters: High blood pressure and cholesterol often have no symptoms but raise your risk for heart disease and stroke.
- When: At least every 1–2 years—or more often if you have risk factors.
✅ Blood Sugar / Diabetes Screening
- Why it matters: Type 2 diabetes is increasingly common in midlife, and catching it early can prevent serious complications.
- When: Starting at age 45, or earlier if you’re overweight or have family history.
✅ Cancer Screenings
- Breast Cancer: Mammograms are recommended for women starting at 40–50, depending on risk factors.
- Colon Cancer: Colonoscopy or stool-based screening should begin at 45.
- Prostate Cancer: Men should discuss PSA testing with their doctor around age 50, or earlier with risk factors.
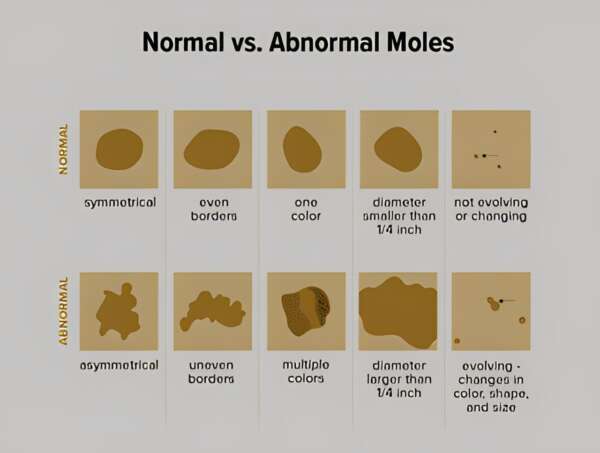
- Skin Cancer: Regular skin checks for unusual moles or lesions are important at any age.
✅ Bone Density Test (DEXA Scan)
- Why it matters: Osteoporosis risk increases with age, especially for women after menopause.
- When: Women over 65 and men over 70 should be screened—but your doctor may recommend earlier if you have risk factors.
✅ Vision & Hearing Checks
- Why it matters: Subtle changes in vision and hearing can impact daily life and safety, yet often go unnoticed.
- When: Eye exams every 2 years; hearing checks if you notice changes.
✅ Immunizations
- Why it matters: Protection against illness doesn’t stop at childhood. Staying up to date reduces serious risks.
- Key vaccines: Shingles (age 50+), annual flu shot, Tdap booster, and COVID-19 vaccines/boosters as recommended.
Why This Matters More in Your 40s & 50s
These decades are often the “sandwich years”—balancing careers, families, and aging parents. It’s easy to put your health last. But screenings are one of the most powerful ways to stay healthy, independent, and present for the people who count on you.
Your Partner in Prevention
At Roots Health DPC, we take the guesswork out of prevention. Together, we’ll create a personalized screening plan based on your history, lifestyle, and risks. With direct access to your doctor, longer visits, and ongoing support, you’ll never feel rushed or overlooked.